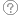Case preparation
What are the different types of abnormal menstruation?
- Absence of menstruation (Amenorrhoea)
- Infrequent periods (Oligomenorrhoea)
- Heavy menstrual bleeding (Menorrhagia)
- Painful periods (Dysmenorrhoea)
- Intermenstrual bleeding and spotting
- Postcoital bleeding
- Postmenopausal bleeding
Amenorrhoea
Absence of menstruation, either primary which means that periods have not started by age 16 years or secondary where periods have stopped for longer than 6 months in a woman who previously had periods.
Causes of Amenorrhoea?
- Physiological - these are common and frequently overlooked. Physiological causes include pregnancy, lactation and menopause
- Hypothalamic / pituitary disorders - inhibition of the hypothalamus can be caused by stress, weight change, excessive exercise and various drugs. Tumours such as prolactinoma or damage to this area e.g. Sheehan's Sydrome can also result in amenorrhea.
- Ovarian anomalies - these include gonadal agenesis (XX or XY ) but phenotypically female or dysgenesis of which Turner's syndrome is the most common (46XO). Other ovarian causes of amenorrhea are PCOS (polycystic ovarian syndrome), premature ovarian failure and of course surgical removal of the ovaries.
- Uterine and outflow tract disorders - these are rare and include congenital anomalies of anatomy such as absent uterus or vagina, cervical stenosis, vaginal septum and imperforate hymen. Outflow disorders can also be caused by damage to the endometrium with adhesions secondary to curettage (called Asherman's syndrome) or from infection by tuberculosis. Androgen Insensitivity Syndrome can also rarely cause amenorrhoea. People with this syndrome are 46 XY with mutations in AR gene, have external female characteristics but do not have a uterus.
- Other endocrine anomalies - occasionally hypo or hyperthyroidism and adrenal abnormalities such as Cushing's syndrome or adrenal tumours can result in cessation of menstruation.
Taking the History.
- You will want to ask the woman whether she previously had periods and the duration of the amenorrhoea. If she has never had periods has there been development of secondary sexual characteristics such as breast development or appearance of pubic hair?
- Is she sexually active/using contraception? Have you considered pregnancy or lactation as a cause of amenorrhoea?
- If periods were present previously, has her weight recently changed? Is she undertaking strenous exercise?
- Has she noticed any symptoms of estrogen deficiency such as hot flushes to suggest that she may be perimenopausal? Or any symptoms of androgen excess such as hirsuitism or acne, which commonly occur in polycystic ovarian syndrome.
- Any headaches, blurred vision, loss of discharge from the breast (galactorrhoea). What might these changes suggest?
Examination.
- Measure the women's weight and height and calculate the BMI
- Check the blood pressure
- Look for signs of hirsutism and acne
- Are secondary sexual characteristics present?
- Ensure there is no palpable pelvic or abdominal mass on abdominal palpation
- If the woman is sexually active, then a pelvic examination should be offered (a pelvic examination should NOT be performed if the woman has not been sexually active)
- If visual concerns or headache is reported, then a visual field examination, fundoscopy and a neurological examination are important as the cause my be a prolactinoma
![]() Activity-What investigations will you do??
Activity-What investigations will you do??
Have a think about what specific investigations you might want to consider for a woman who presents with amenorrhoea -a quick look again at the causes we have just discussed will help give you the answers. Make a list of these investigations - now compare that with our answer .
Click here to compare your list with ours
- Pregnancy test
- Gonadotrophin levels eg LH, FSH
- Prolactin level
- If signs or symptoms of thyroid disorder then do thyroid function tests (TSH)
- Androgen screen (free testosterone)
- Pelvic or vaginal ultrasound
Oligomenorrhoea- Polycystic ovarian syndrome (PCOS)
The most common causes of amenorrhoea or oligomenorrhea is polycystic ovarian syndrome (PCOS). It is also the commonest endocrine disorder in women. You will learn more about PCOS in Case 13. It is important to differentiate between only seeing a polycystic appearance of the ovary on an ultrasound scan (USS) and the syndrome as about 20-30% of women of reproductive age will have the appearance of polycystic ovaries on ultrasound but the prevalence of the syndrome is less: Around 5 to 10%. This is an important distinction as it is the Syndrome that may be associated with other adverse health outcomes such as increased risk of Type 2 Diabetes, obesity and endometrial hyperplasia and carcinoma.
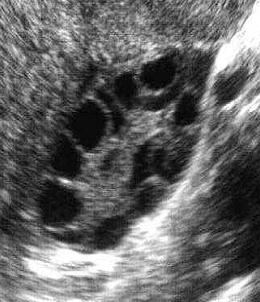
The USS appearance of polycystic ovaries. Note the characteristic "string of pearls" appearance of the multiple "cysts" (follicles) on the surfact of the ovary. These cysts are tiny, less than 1cm, and are quite different from other ovarian cysts that you may read about.
So how do we define and diagnose Polycystic Ovarian Syndrome?
The definition of PCOS has been evolving for many years and a single finding does not permit diagnosis. The current definition (known as the Rotterdam definition) requires the presence of any 2 of the following 3:
- Oligo and / or anovulation which commonly manifest as oligomenorrhea or irregular and unpredictable bleeding pattern.
- Clinical (hirsuitism,acne) and /or biochemical (raised free testosterone) evidence of androgen excess (hyperandogenisation)
- Polycystic ovary/ies on transvaginal USS- 12 or more follicles in either ovary measuring 2-9mm in diameter and/or increased ovarian volume >10ml
Menorrhagia
Menstrual problems are a common reason for referral to gynaecology clinics. In 1997 about 80% of the hysterectomies in New Zealand were performed for heavy menstrual bleeding (HMB) and about one in five New Zealand women had had a hysterectomy by age 50. You will learn more about HMB in Case 12. This high surgical rate was one of the reasons for producing the NZ Guidelines on Heavy Menstrual Bleeding in 1998. Options for medical treatment may include hormonal and non-hormonal medications, which may be given orally or as an injection, in the case of Depo Provera. The Mirena IUS is an intrauterine contraceptive device that releases progesterone and is increasingly used in the effective treatment of menorrhagia as well as dysmenorrhoea. The introduction of the Mirena has significantly reduced the number of hysterectomies that were previously performed for menorrhagia and they can remain in situ for 5 years. Surgical treatments include hysterectomy (a major operation, achieved by either the abdominal or vaginal route) or endometrial ablation. An important part of discussing management options with patients involves asking about treatments she has tried, identifying a possible underlying cause, understanding the patient’s current and future fertility plans (does she desire a future pregnancy?) and enquiring about any other symptoms she may have, such as dysmenorrhoea (see later).
Heavy periods can also be caused by systemic problems such as platelet, coagulation and thyroid disorders. However we would not routinely check TFTs or do coagulation screen unless there were other signs or symptoms of problems in these areas. The commonest cause of heavy periods is dysfunctional uterine bleeding (ovulatory or nonovulatory). Other common causes may be structural causes such as fibroids and endometrial polyps.
Occassionally, women can present acutely with menorrhagia or with symptoms of severe iron deficiency anaemia because of chronic, or less commonly, acute blood loss. Symptoms of anaemia may include fatigue, breathlessness on exertion, dizziness and palpitations. The woman may be pale and tachycardiac on examination. It is important to make sure that she is haemodynamically stable (that her blood pressure and pulse are normal) and that she does not need intravenous fluid resuscitation. In some situations, it may be necessary to offer blood transfusion if the haemoglobin is significantly low and/or the woman is symptomatic. It will then be necessary to implement measures to try to reduce the amount of bleeding if she is currently menstruating and this is usually achieved through the use of high dose provera (progesterone) and tranexamic acid, before other long term management options, as you will discuss below, can be considered. Many women will need to also be on an oral iron supplement.